Quantifying Matters of the Heart: Using Mathematical Modeling to Simulate Vital Organs
Songwriters, poets, and novelists have long tried to capture the intricacies of the heart. But it’s the quants who might finally do it.
The Living Heart Project, initiated by the firm Dassault Systémes, is applying the advanced technology that the automotive and aerospace industries use to realistically simulate the heart. The project has solicited input from cardiovascular researchers, biopharmaceutical companies such as Pfizer, regulatory agencies and practicing doctors to develop a model heart. The result is a realistic organ that scientists can experiment on, without harming a soul.
The result isn’t merely a more detailed version of the plastic 3-D organs a high school science teacher might have on display. The simulations incorporate what science knows about the structure and function of the heart, down to the minutiae. Using supercomputers, a heart can be “rebuilt” from scratch to test out different scenarios.
“You can create many different cells, and each cell has a function that connects to other cells, so you can get the full dynamic simulation of a beating heart,” says Cynthia (CJ) Musante, Senior Scientific Director at Pfizer. “Each cell in the simulation follows its own mathematical model. Then it interacts with the other cells around it.”
Not Just a Model — A Supermodel
Dassualt’s long-term plan is to adapt the simulation to specific patients’ hearts. “Hypothetically, let’s say you’re having a heart problem,” says Musante. “You would get an MRI and they can create a computer representation from those images. They could then build a mathematical model and do simulations of your heart,” testing different medications or surgical options to see which would be best.
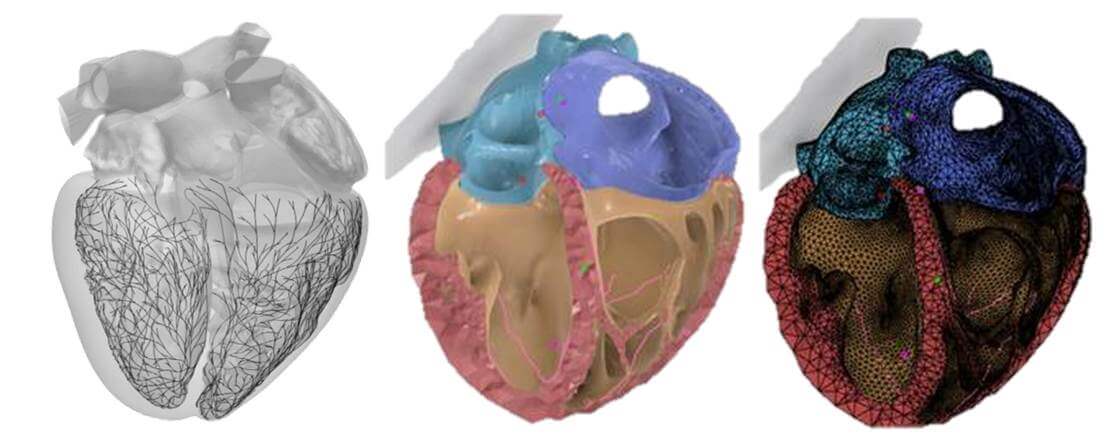
Visual depictions of various cardiac function models. Modeling the Purkinje network (left), the heart’s electrical pathway, is crucial because it drives the heart to beat, which in turn, moves oxygenated and deoxygenated blood through your heart. The Solid Model (middle) is a virtual representation of the Purkinje network in the Living Heart, which is converted to a Finite Element representation (right) that is used in simulation analyses to understand pharmaceutical toxicity on the heart, RadioFrequency ablation treatment efficacy, and medical device safety and performance. (Courtesy Dassault Systémes)
The Living Heart could help pharmaceutical researchers see the effect of a medication at a cellular level “and then we could see how that would propagate to the whole heart,” says Musante. “It would be different in a patient who had heart failure, for example, so we could see how the structural components like the fibers of the heart would change in that case. It could help us make design decisions about clinical trials.”
Part of a Larger Trend
The Living Heart Project is part of a greater movement to create realistic models of vital organs in order to invent new and better medical devices, improve surgical techniques and design more targeted medicines. In the US, the FDA is even using these 3D models in some evaluations of potential medicines and devices.
In Switzerland, the Blue Brain Project is working on digital reconstructions and simulations of the human brain. Starting with the rodent brain, the project is building models with an unprecedented level of biological detail. And in Germany, the government has invested in a program called the Virtual Liver Network, which is attempting to integrate the wealth of data available about the liver into a series of models that will represent how the organ functions.
Here in the US, Musante runs the Quantitative Systems Pharmacology Lab at Pfizer. “We engage with a lot of researchers and groups who are building these models, like Dassault,” she says, “and we build our own models to try to address mechanistic questions and better understand diseases.”
