What are the symptoms of eczema?
Find the answer to this question and ask more at Health Answers by Pfizer.
![]()
Atopic Dermatitis is one of the most common chronic inflammatory skin conditions, affecting people of all ages and genders around the world.1 It is not contagious. Symptoms tend to wax and wane and can vary widely in severity from person to person.1,2 The most frequent eczema symptom is itchy skin, but people with eczema can also experience dry skin, rashes, scaly patches, oozing lesions, and secondary skin infections.2,3 Atopic dermatitis is the most common form of eczema, and sometimes the terms are used interchangeably.2,3
Eczema affects more than 31 million Americans.3 Prevalence is highest in early childhood, with as many as 20% of children experiencing eczema at some point.1,2 Symptoms typically appear before age 5, but children of any age and adults can develop eczema.2 The condition affects approximately 7% of adults, and roughly 40% of patients experience moderate to severe symptoms.4 Although eczema is increasingly common among older adults, it is less common to begin experiencing symptoms after age 60.4,5
In the United States, the prevalence of atopic dermatitis among children has increased over the past two decades. Atopic dermatitis affects children at similar rates no matter their gender, but among adults, it is slightly more prevalent in people assigned female at birth.4 Atopic dermatitis is also more prevalent among African Americans than European Americans in the US.6 Additionally, research indicates that Black, Hispanic, and people with low income levels may experience a greater burden managing eczema, including disparities in health literacy and access to quality healthcare.7

Eczema is caused by a mix of environmental and genetic factors, but the exact causes are unknown.8 The condition is often associated with asthma and other allergic diseases, such as food allergies and hay fever.9 People with eczema tend to have an altered immune system activity that can lead to inflammation.8 Research also points to a possible connection between eczema and a mutation of the filaggrin gene, which is responsible for producing a protein that helps maintain a healthy outer skin barrier. A deficiency in this protein can affect the skin barrier, which can result in decreased moisture of the skin and increased exposure to viruses, bacteria, and allergens, allowing them to enter the body and trigger a hyperimmune response.8,10
Genetic risk factors for this skin disease include having a family history of eczema, asthma, hay fever, or food allergies.9 Environmental risk factors for eczema may also include living in places that are cold and damp or hot and swampy for at least some of the year.8
Many different triggers can cause or worsen eczema flare-ups, such as exposure to pet dander, dust mites, household products or products with heavy fragrances. Other triggers can include stress, hot or cold climates, sweating, skin contact with irritating chemicals or rough materials, excessive hand washing with soaps, or bathing excessively without moisturizing properly afterward.8,9,10,11
There are no known cures for eczema, but patients can try to avoid known triggers of eczema to help control their symptoms.12 For example, people with eczema might benefit from managing stress, properly taking care of their skin, and eating an eczema-sensitive diet.8 It may help to moisturize regularly, choose products without a heavy fragrance, wear loose-fitting, cotton clothing (avoid rough fabrics like wool), and minimize exposure to pet dander, dust mites, and other potential environmental triggers.8,13
Atopic dermatitis is a common skin disorder that causes itchy skin and rashes, which can be painful and interfere with sleep and day-to-day life.14
Contact dermatitis occurs when an allergen or irritant comes in contact with the skin, causing a reaction that can include itchy skin, rashes, and/or blisters.15
Seborrheic dermatitis is a chronic form of eczema that affects parts of the body that have many oil-producing glands, such as the scalp, face, mid-chest, and upper back, causing dandruff and/or rashes in affected areas.16
Stasis dermatitis, also known as gravitational dermatitis, venous stasis dermatitis, and venous eczema, results from poor circulation in the lower legs, also known as venous insufficiency. It most often affects people older than age 50 and, in some cases, can be a sign of more serious underlying medical issues.17
Nummular eczema causes round, itchy patches, usually on hands, lower legs, or forearms. It tends to result from extremely dry skin or can develop in people who have other rashes, including atopic dermatitis.18
Dyshidrotic eczema, also known as pompholyx, causes very itchy blisters on the hands or feet. It can be a one-time experience or chronic. Although symptoms may look contagious, dyshidrotic eczema, like all forms of eczema, isn’t spread from person to person.19
About 60% of people with eczema will develop symptoms by the age of 1, and 30% more will see symptoms by the age of 5.2 Parents of children with eczema may wish to consult a pediatrician, allergist, or dermatologist for guidance on managing flare-ups.2,20
Eczema appears and behaves in different ways depending on a child’s age. Newborns tend to experience red, “weepy”-looking symptoms on their face, chin, cheeks, scalp, and/or forehead. Babies older than six months might experience rashes on their elbows and/or knees, often due to friction from crawling. Toddlers with eczema may experience dry, scaly skin on their inner elbows, inner knees, wrists, hands, or ankles, or around their eyelids and mouth. Children older than 5 may experience eczema symptoms on their hands, feet, and/or scalp, on the inner side of the elbows or knees, or behind their ears.20
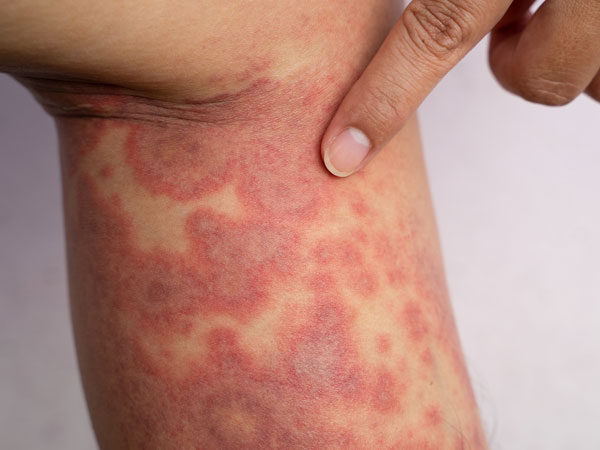
Eczema symptoms range from mild to severe and can affect some people on a daily basis, potentially causing intense discomfort that can disrupt sleep. Symptoms can include red rash, itchiness, and dry skin that can crack, bleed, and/or ooze. In infants and toddlers, eczema symptoms often appear on the cheeks or on the outsides of elbows and knees. In older children and adults, eczema is most common on the hands, feet, arms, and backs of knees.1,2 Eczema can also develop on the eyelids and skin around the eyes and may also increase the risk of developing diseases of the eyes themselves, affecting one’s vision.21
Patients with atopic dermatitis can experience worsening symptoms because of heightened allergic responses to environmental irritants, such as pollen or dust mites. Patients might also experience exacerbated eczema symptoms as a result of developing hypersensitivity to metals, such as cobalt or nickel.5
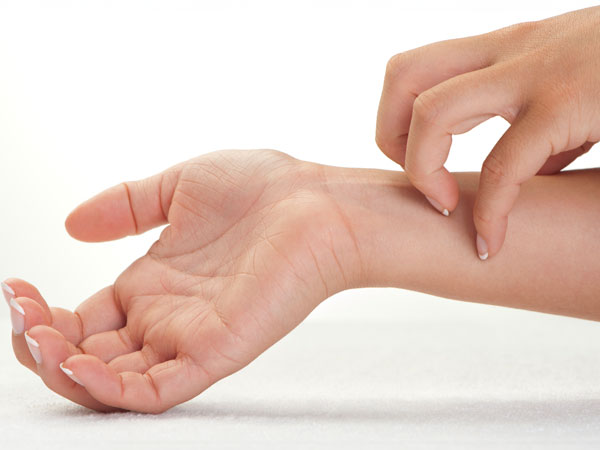
People with atopic dermatitis are vulnerable to bacterial and viral infections, which, in turn, can worsen their atopic dermatitis symptoms.22 A similar self-perpetuating cycle can occur with itching. In this so-called ‘itch-scratch cycle’, itching leads to scratching, which temporarily relieves pain but ultimately leads to more intense itching.14,23 Excessive scratching can cause scarring or be associated with neurodermatitis, a disorder in which affected skin becomes leathery, thick, and very itchy.23
In some cases, discomfort from eczema and its impacts on daily life can cause or exacerbate emotional and mental health issues for patients and caregivers.1
There is no laboratory test for diagnosing atopic dermatitis. Instead, it’s a clinical diagnosis. About 80% of people with atopic dermatitis will receive their diagnosis and treatment from a primary care provider.10
The National Eczema Association (NEA) recommends keeping fingernails short and filed smooth to help reduce damage from scratching. But the organization also notes that it’s important to limit scratching as much as possible.23
The American College of Allergy, Asthma, and Immunology (ACAAI) offers several specific recommendations for managing eczema and reducing risk:2
For some chronic eczema issues, home remedies can be helpful. The National Eczema Association suggests:2,3,10,23
Menthol and calamine lotion and over-the-counter corticosteroids can reduce mild itchiness, according to the National Eczema Association. Unfortunately, antihistamines don’t work for eczema the way they do for skin allergies and other conditions that cause skin damage. However, the NEA notes that antihistamines may cause drowsiness, which may help people with eczema sleep better.23
For moderate to severe cases of eczema, a dermatologist or allergist might prescribe topical treatments known as antipruritics or topical anesthetics to reduce itch. They may also prescribe oral antibiotics for skin infections.12,23 People with eczema might also be prescribed steroids, topical calcineurin inhibitors, or other medications. For atopic dermatitis patients with moderate to severe symptoms, injectable biologic medications may be available. When other medications fail to manage symptoms, healthcare professionals may prescribe other advanced treatments targeting cells in the immune system thought to be associated with eczema. In some cases, healthcare professionals may suggest phototherapy, also known as light therapy. Phototherapy uses specific wavelengths of ultraviolet light to treat eczema.12

Atopic dermatitis costs Americans approximately $5 billion annually, based on direct and indirect costs, including medication and, especially for people with severe symptoms, reduced productivity and quality of life.4 Eczema symptoms are associated with impaired concentration and lost workdays for adults and lost school days for children.4,14 Research indicates eczema creates a global burden, particularly in high-income regions and resource-rich countries, possibly because improved hygiene and living conditions can have the unintended consequence of triggering eczema flare-ups.24
Eczema is caused by a mix of environmental and genetic triggers, but the exact causes are unknown.8
Eczema and psoriasis are different conditions with key distinctions, but they’re easily mixed up. Both involve an overactive immune system and can result in itchy skin. Both can be hereditary and triggered by a variety of environmental factors. But psoriasis causes the immune system to trigger the rapid growth of skin cells, causing thick plaques or scales to form on the surface of the skin. Eczema, in contrast, results in inflammation and impaired skin barrier.1,25
In the United States, eczema is approximately four times more prevalent than psoriasis. Eczema can affect people of all ages, but symptoms often emerge at young ages. In contrast, people usually develop psoriasis symptoms between the ages of 15 and 35.25
Although there is no known cure for eczema, people with eczema can use lifestyle adjustments and home remedies, over-the-counter, or prescription treatments to manage symptoms. Your doctor might recommend topical therapies, such as applying moisturizers to the skin, topical medicated therapies, or systemic therapies, taken by pill or injection.3,12 In some cases, UV light therapy, or phototherapy, may help manage eczema symptoms by treating the condition with professionally monitored ultraviolet light.12,26
Yes, atopic dermatitis affects as many as 25% of children in the U.S., and about 60% of patients with eczema experience symptoms before turning 1 year old.27
Some of the most common types of eczema include atopic dermatitis,14 contact dermatitis,15 seborrheic dermatitis,16 stasis dermatitis,17 nummular eczema,18 and dyshidrotic eczema.19 These various forms of eczema typically cause symptoms such as itchy skin, rashes, or oozing skin, sometimes resulting in pain and interferences with daily life.14,15,18
The skin disorder is pronounced “eg-zuh-MUH.”3
No, eczema is not contagious.8
Eczema can be chronic, meaning symptoms can persist into and through adulthood. But some children who experience eczema may outgrow symptoms.2
Some products that don’t require a prescription might be enough to manage your child’s eczema, as well as some at-home remedies such as daily bathing followed by immediate moisturizing.2 But for more persistent symptoms in children, it might be wise to consult a dermatologist or allergist.2,27
Yes, adults can get any form of eczema. Atopic dermatitis that emerges after a person turns 18 is often called “adult-onset atopic dermatitis.” Atopic dermatitis symptoms can also fade away during childhood and then reappear in adulthood.28
No, there is no known cure for eczema, but there are many ways to help manage symptoms and reduce the pain and itchiness associated with them.8
Find a Pfizer clinical trial for eczema at PfizerClinicalTrials.com.
Explore eczema clinical trials at ClinicalTrials.gov.
Area of Focus: Inflammation & Immunology
Eczema is a focus of Pfizer’s Inflammation & Immunology Therapeutic Area. Visit the Inflammation & Immunology Page.
The information contained on this page is provided for your general information only. It is not intended as a substitute for seeking medical advice from a healthcare provider. Pfizer is not in the business of providing medical advice and does not engage in the practice of medicine. Pfizer under no circumstances recommends particular treatments for specific individuals and in all cases recommends consulting a physician or healthcare center before pursuing any course of treatment.