What are the different types of psoriasis?
Find the answer to this question and ask more at Health Answers by Pfizer.
![]()
Psoriasis is a chronic condition in which the body's skin cells grow too quickly. Instead of shedding, the skin cells build up on the surface of the skin and cause plaques or raised patches of rough skin. Psoriasis can burn, itch, and sting.
Psoriasis is caused by an overactive immune system that leads to inflammation and a shorter skin cell growth cycle. Plaques commonly occur on the elbows, knees, back, face, palms, feet, and scalp, but they can show up anywhere.1,2
Psoriasis most often affects people between ages 15 and 35.2 At least 8 million U.S. adults have psoriasis.3
Psoriasis can look like other skin conditions, such as eczema. Both cause itchy, inflamed skin, but they have different causes. Psoriasis and eczema can occur in people of any age, but eczema mostly affects babies and children while psoriasis most often affects adults.4
Eczema patches tend to be thinner with less-defined borders than plaque psoriasis. In some locations, such as the palms or soles of the feet, both conditions can look similar. Itching is more common with eczema while pain is more common with psoriasis.4 It's important to see a dermatologist for an accurate diagnosis because eczema and psoriasis require different treatments. A dermatologist may remove a bit of skin and examine it under a microscope to make a definitive diagnosis.2
The exact cause of psoriasis isn't known, but it's thought to be caused by a combination of genetics and environmental factors. Psoriasis is most common in people with white or light-colored skin, but it can occur in anyone. It affects all genders equally.5
The immune system plays a role in psoriasis. Normally, skin cells grow and shed, a process that takes about a month. With psoriasis, this process happens in a few days, causing skin cells to build up on the surface.1,6
Researchers have learned that this happens quickly because the body's T cells, which are a part of the immune system, attack skin cells. But they don't know exactly why this happens. When the immune system overreacts like this, it tends to continue for the rest of a person's life.7

Psoriasis is not contagious and there aren’t clear risk factors, but people can experience triggers that cause flare-ups. Triggers vary by individual but include:2,5,7
Psoriasis often runs in families. Someone with a parent, grandparent, or sibling who has psoriasis is more likely to develop the condition. However, the connection between genetics and psoriasis is unclear.7
Researchers have found that some genes occur more frequently in people with psoriasis. But not everyone who develops psoriasis has those genes.7 Scientists think that people must experience certain triggers before psoriasis develops regardless of genes.7
Children can develop psoriasis, but it's much less common in children than adults. One exception is guttate psoriasis. This type often appears after strep throat or another infection and clears up on its own.4,8
Psoriasis in children can look like a yeast infection, diaper rash, or cradle cap. It can also be confused with eczema.8
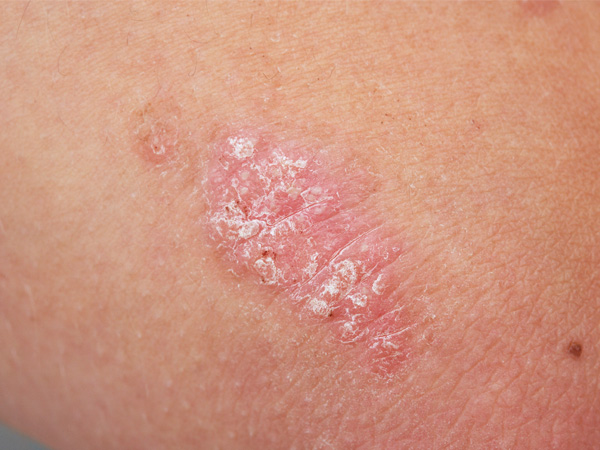
The most common type of psoriasis is plaque psoriasis, which causes raised, scaly patches of skin that tend to have defined borders. On light-colored skin, the patches may look red with silvery-white scales. On darker skin, these patches may look red, brown, or purple.6,9
This type of psoriasis causes tiny, scaly pink bumps. They commonly show up on the torso, legs, and arms but also appear in other areas.6,9,10 It usually occurs in children or young adults after an infection such as strep throat.
Accounting for about 2% of all psoriasis cases, guttate psoriasis often appears and clears up without treatment. However, it is possible to develop chronic guttate psoriasis, and some people who get it develop plaque psoriasis.6,8,9,10
Inverse psoriasis occurs in less easily visible areas, where skin touches skin, such as the armpit or genitals or under the buttocks or breasts. It tends to present as sore, red skin that looks smooth and shiny.9,11
Pustular psoriasis occurs most often on the feet or hands. It appears as pus-filled bumps. The bumps are not an infection, but the skin can feel sore or painful.11,12
This is a rare but life-threatening form of psoriasis that causes large portions of the body to appear burned.11,13 A person may experience chills, fever, heart rate increases, and severe itching.13 Anyone with erythrodermic psoriasis should seek immediate medical attention.11
Signs of psoriasis vary by person and by type of disease. The most common psoriasis symptoms include: 2,5,9
Common signs of psoriasis are most often found on the elbows, knees, and scalp, but psoriasis can also develop on the hands, nails, face, genitals, or feet.1,9
Psoriasis is most common in people with white or light-colored skin, but it can occur in anyone. For people with darker skin, plaque psoriasis may appear darker red or brown, purplish, or even grayish, and patches may be thicker. People of color who have psoriasis tend to have more severe cases that cover more of their bodies.9,14
People with psoriasis are at higher risk of developing other complications, emphasizing the need for ongoing disease management. Researchers have found connections between psoriasis and diabetes and kidney disease, among other conditions. People with psoriasis are at increased risk of developing:5

A dermatologist diagnoses psoriasis through a physical exam and by looking at a bit of skin under a microscope. Then the dermatologist works with the patient to develop a treatment plan based on the type of psoriasis, its location on the body, and its severity.
Psoriasis cannot be cured, but treatment helps keep it under control and manages symptoms. Following a treatment plan can help reduce the risk of complications and related health conditions.
Because it is a chronic condition, psoriasis can worsen over time, requiring changes to the treatment plan. A dermatologist can recommend how to treat psoriasis at each stage of the disease and the best products to use.2,6,15
Creams that contain hydrocortisone or coal tar are among the most common treatments for mild psoriasis. Over-the-counter creams, gels, and ointments work for some people while others need prescription-strength topical creams.2,16
Products with salicylic acid can also help remove scales. Moisturizers can help control dryness and allow the skin to heal.16
Topical treatments like creams may also be used to treat nail psoriasis or psoriasis on or around the genitals.17,18
Some people need to take medication in the form of pills, liquids, or injections to control psoriasis symptoms:2,19
Biologics for psoriasis include:20
Light therapy for psoriasis exposes the skin to ultraviolet light and can be done at home or in a doctor's office or clinic. Ultraviolet light B (UVB) is than effective way to slow the growth of skin cells. People receiving therapy undergo exposure to a UVB light source for a prescribed amount of time.21 People with psoriasis should not use tanning beds and should talk with a doctor about sun exposure and sun protection.
In addition to physical challenges, psoriasis can affect people's social and emotional well-being. Some people may feel a stigma or embarrassment about their skin. It's important that people with psoriasis find a support system.14
As psoriasis lesions clear, dark or light spots on the skin can remain. These changes in pigmentation can appear more obvious on people with darker skin. A dermatologist may be able to prescribe creams or ointments to address these. Over time, the spots may clear up, though some may always remain.14
Psoriasis often flares up and then subsides. Learning what triggers flare-ups and avoiding them helps keep symptoms under control.22
Cold or hot weather can cause flare-ups for some people. Moisturizing more frequently in the winter or avoiding sun exposure can help. Skin damage is another common trigger, with psoriasis sometimes flaring up after shaving or getting tattoos, piercings, scrapes, or bug bites.22
Adopting regular physical activity helps maintain a healthy weight and reduces the risk of psoriasis complications, such as diabetes, fatty liver disease, unhealthy cholesterol levels, high blood pressure (hypertension), and heart disease. Exercise may also help maintain a healthy weight, reducing the risk of the aforementioned diseases, as well as reducing stress, depression, and anxiety.23
Smoking or frequent exposure to secondhand smoke can also cause psoriasis to flare unexpectedly. Nicotine patches may irritate the skin, so a doctor can advise about th e best methods to quit smoking.22
There's no diet that’s specific to people with psoriasis, but following a healthy eating plan can help reduce the risk of conditions that often occur alongside it. Choose a diet with fruits and vegetables, lean meat or fish, and low-fat dairy products. Limit sodium intake and keep processed foods to a minimum.24
People who notice flare-ups after eating certain foods should avoid those foods.24
Excessive drinking can also cause flare-ups. More than two alcoholic beverages a day can worsen psoriasis despite taking medications. Additionally, alcohol can interfere with the effectiveness of some medications.22
Psoriasis and stress appear to be linked, with many people reporting flare-ups when they're stressed. Finding ways to reduce stress, such as practicing yoga or mindfulness, can help keep symptoms under control.22
The World Health Organization considers psoriasis a serious global problem.25 About 125 million people worldwide have psoriasis, and psoriasis is more prevalent in high-income countries.3,26 As of 2020, 3.6% of white people have the disease compared with about 1.5% of Black people. However, psoriasis may be underdiagnosed in people of color because the condition looks different on darker skin.3
Psoriasis contributes to healthcare costs of $135 billion annually in the United States and affects people's mental, emotional, and social well-being.3
Psoriasis, particularly moderate and severe disease, can affect a person's quality of life, leading to disability, social stigma, and isolation.14

Yes. Issues in the immune system lead to psoriasis. Normally, cells grow deep in the skin and rise to the surface over the course of a month. With psoriasis, skin cells rise too quickly over the course of days.1
The connection between psoriasis and genes isn't clear. Psoriasis runs in families, and researchers have found that people with psoriasis are more likely to have certain genes. However, not everyone with the genes gets psoriasis, and some people without the genes can also develop the disease.7
Itching is a common symptom of psoriasis, and scratching can cause skin damage, making the condition worse. Applying anti-itch creams can reduce the urge to scratch.2,16,22
Plaque psoriasis is the most common type and looks like raised patches of thick skin with silvery-white scales on top.11 In people with fair skin, the patches often look red. In people with darker skin, they can look brown, purple, or grayish.14
Psoriasis cannot be spread to other people.2
Find a Pfizer clinical trial for psoriasis at PfizerClinicalTrials.com.
Explore psoriasis clinical trials at ClinicalTrials.gov.
Area of Focus: Inflammation & Immunology
Psoriasis is a focus of Pfizer’s Inflammation & Immunology Therapeutic Area. Visit the Inflammation & Immunology Page.
The information contained on this page is provided for your general information only. It is not intended as a substitute for seeking medical advice from a healthcare provider. Pfizer is not in the business of providing medical advice and does not engage in the practice of medicine. Pfizer under no circumstances recommends particular treatments for specific individuals and in all cases recommends consulting a physician or healthcare center before pursuing any course of treatment.