What is lupus and how does it affect the body?
Find the answer to this question and ask more at Health Answers by Pfizer.
![]()
Lupus is a chronic autoimmune disease that causes inflammation as the immune system attacks healthy tissue all over the body. It primarily affects the skin, joints, and internal organs such as the kidney and heart. However, since it can impact many different areas of the body, symptoms vary widely.1
The Lupus Foundation estimates that about 1.5 million Americans and at least 5 million people around the world have some form of lupus. The disease primarily impacts those assigned female at birth (90%) during childbearing age, but those assigned male at birth, as well as children and teens, can develop the condition, too.2
A 2021 epidemiologic breakdown by racial and ethnic subpopulations in the United States demonstrates the prevalence of systemic lupus erythematosus (SLE), the most common form of lupus. In the study:3
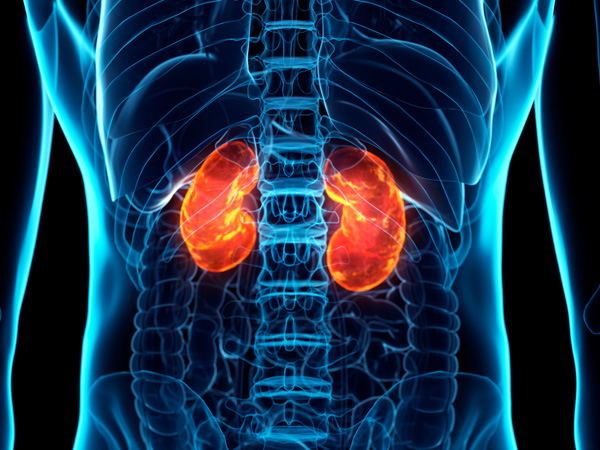
Researchers haven’t identified the cause of lupus. But it's believed that this complex disease is linked to the interactions of hormones, genes, and environmental factors.4
More research is required to determine whether lupus is hereditary. A genetic link first gained attention because of lupus's tendency to cluster in families and show up more frequently in certain ethnic groups.1,4
Genes associated with the disease include:
Hormones and environmental factors may increase a person’s risk of getting lupus. For example, the higher incidence of lupus among those assigned female at birth is believed to be tied to higher quantities of estrogen, thanks to the hormone's "immune-enhancing" characteristics.4 Additionally, genes involved in innate immunity are linked to the X chromosome.6,7
Environmental factors have been elusive, but researchers have discovered connections between lupus and a range of toxins and infectious diseases, including:
Other factors with the potential to aggravate symptoms include certain drugs, ultraviolet light exposure, and stress.4
Lupus is the parent category for several more specific types of this disease.1
Most frequently, people are referring to SLE when they say “lupus.” This type of lupus gets its name from its potential to affect multiple organ systems in the human body, including the joints, skin, and kidneys. It can also extend to the cardiovascular and nervous systems.9
One of the most serious complications of SLE is lupus nephritis, which describes an immune system attack on the kidneys, leading to inflammation and the possibility of organ damage.10 Left untreated, symptoms can worsen and lead to kidney failure. If the condition becomes very serious, a patient may need dialysis or a kidney transplant.11
CLE affects only the skin. Although the disease can occur in people without SLE, at least 5% of people who develop CLE may develop SLE at a later time.1,9
CLE consists of several sub-types. Acute cutaneous lupus erythematosus (ACLE), subacute cutaneous lupus erythematosus (SCLE), and chronic cutaneous lupus erythematosus (CCLE), which is also called discoid lupus erythematosus (DLE), are the most common.12,13
ACLE can be localized (occurring on one part of the body) or generalized (occurring on multiple parts). In localized form, ACLE typically takes the form of the butterfly rash (or malar rash). The rash’s duration can range from days to weeks, and sun exposure may cause it.13
Like ACLE, SCLE is often triggered by sun exposure. But unlike ACLE, the rash typically occurs on upper parts of the torso and on the neck, back, and arms—not the face.13
CCLE is also called discoid lupus erythematosus (DLE), and it is one of the most frequently encountered types of cutaneous lupus. DLE is a chronic skin condition that presents as sores with inflammation and scarring. It typically shows up around the face, ears, and scalp, although it can appear in other areas. The lesions are red, inflamed patches that appear thickened . The condition can cause permanent scarring and hair loss.13
Childhood lupus mirrors the effects of the adult form of the condition. But unlike adult lupus, childhood lupus is more common in those assigned male at birth. Childhood lupus also affects certain organs more significantly, including the kidneys. Children diagnosed with lupus develop kidney disease twice as often as adults with lupus.9
NLE occurs when a mother transfers autoantibodies of Sjogren syndrome to an unborn baby. Those autoantibodies include autoantigen type A (Ro/SSA) or autoantigen type B (La/SSB).14 These antibodies occur in about 1 in 1,000 healthy individuals, meaning that a pregnant person who has a child with neonatal lupus may not have the disease themselves.9 Although rare, NLE can include rashes and cardiac issues.9,14
While the general cause of lupus is unknown, some drugs can trigger lupus-like symptoms, even in people who don't have SLE. Unlike other types of lupus, drug-induced lupus erythematosus is transient. Discontinuing the drug causing the condition usually resolves the rash in a matter of months. Additionally, doctors are increasingly avoiding medications known to induce lupus.9
These medications include:9
Part of the challenge of diagnosing lupus is that its symptoms vary. They may fluctuate over time during and between flare-ups. Symptoms range from mild to severe and may affect just one area of the body or multiple systems at a time. Symptoms often show up alongside the disease-causing inflammation of particular organs such as the skin, lining of heart and lungs, kidneys, joints, brain, and even blood cells.18
SLE diagnostic criteria can include:19
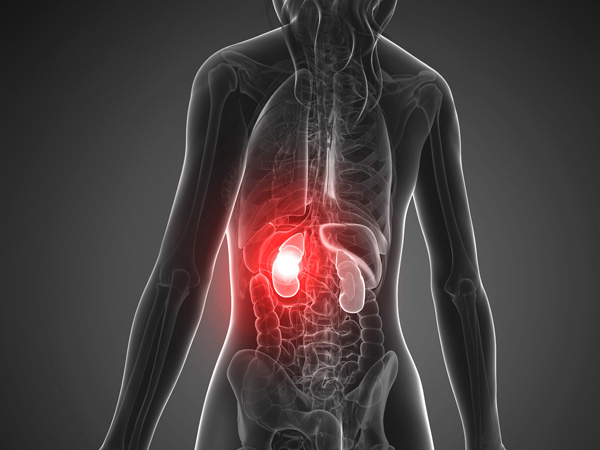
Because lupus promotes inflammation in the body, it can also cause other health issues, including:
Lupus may increase a person’s chances of developing other conditions. For instance, inflammation of tissues in the heart and blood vessels may encourage cardiovascular disease, which can then cause atherosclerosis, or plaques in the blood vessels, as well as coronary artery disease, or plaques in the arteries directly near the heart.18
Less common symptoms include fainting spells, memory loss, and diminishing cognitive abilities. Because none of these signs indicate lupus on their own, they are evaluated within the context of other symptoms to determine whether someone might have lupus.25
Although lupus is more common among those assigned female at birth, those assigned male at birth who have lupus are more likely to have serious symptoms, including kidney, heart, lung, and blood issues, as well as antiphospholipid antibody syndrome and pain while taking deep breaths (pleurisy from serositis ). There is minimal research into how lupus affects transgender and nonbinary people, but it is believed that exogenous hormone therapy (such as estrogen therapy) could affect the condition.26
Lupus disproportionately affects people of color. For example, in people assigned female at birth, lupus occurs three times as often in African American people than in white counterparts.27 People of color are also at heightened risk for severe cases of SLE. Black people face higher mortality rates and earlier lupus deaths compared with white people.28
Lupus is difficult to diagnose because its symptoms are often mistaken for those of other diseases. As a result, many people have lupus for a long time before receiving a formal diagnosis.15
There is no single test for lupus, so diagnostic criteria are broad. However, there are ways of determining a patient's status:
This involves talking to a doctor about symptoms and other associated problems. Noting symptoms, especially highlighting when and for how long they occur, is useful.15
Doctors will want to know if a patient has a family history of lupus or other autoimmune diseases.15
In a physical exam, a doctor will look for rashes or other symptoms associated with lupus.15
As an initial blood test , an antinuclear antibody (ANA) test can show whether a patient's immune system is more likely to create lupus autoantibodies. While most people with lupus have a positive test for ANA, a positive result doesn't mean someone definitely has lupus. After a positive test result, a doctor will order more tests for antibodies that are specific to SLE and may conduct urine tests to screen and monitor for kidney dysfunction.15,16
Coagulation tests are used to identify the lupus anticoagulant. If lupus anticoagulant is present, the blood will take longer than normal to clot during the coagulation test. The lupus anticoagulant is a type of antiphospholipid (APL) antibody, which roughly half of all lupus patients have, making APL useful in the initial diagnosis of lupus. Other APL tests include anticardiolipin antibody and anti-beta2 glycoprotein 1.15,17
This method involves minor surgery to obtain tissue samples. These samples are then examined under a microscope to look for signs of autoimmune disease.15
Lupus is difficult to diagnose, and symptoms can change over time. People living with lupus and their loved ones may, therefore, experience uncertainty and frustration. However, in some cases, treatments are available to help manage the disease and promote a higher quality of life . Most lupus treatments are the same regardless of gender or sex.26
Finding a healthcare provider who listens to patient concerns is critical in treating lupus. Most patients will see a rheumatologist, but many people see other specialists as well if they experience damage to specific organs.29
Lupus patients and their caregivers will work with physicians and other clinicians to develop the best treatment plan and outcome goals. The goals of this plan, in addition to general healthcare, will often include:29
Determining the right combination of medicines that best control patient symptoms can take months or longer.29 Currently, there are a handful FDA-approved medications for treating lupus:
Doctors will often prescribe other medications off-label as part of the normal standard of care.34,35 Some of these treatments include:29,34,35
Additional medical treatments also include therapies such as diuretics, anticonvulsants, antibiotics, and bone-strengthening drugs to combat osteoporosis.29
Since lupus is a systemic disease, strong nutritional habits as part of a treatment plan may optimize a patient's overall health.36
It’s recommended that people who have lupus eat a healthy, balanced diet, limiting the consumption of highly processed foods. The Lupus Foundation of America provides tips for eating healthy for those who have lupus.37
Patients with lupus may experience weight gain or loss as their appetite, dietary habits, possible use of steroids, energy levels, and mobility all change. Those with lupus who are between the ages of 35 and 44 and were assigned female at birth have a heart attack risk that's 50 times greater than the risk in the general population, underlining the benefits for them in particular of a diet lower in saturated fats, cholesterol, and sodium.36
Some drugs used to treat lupus, including corticosteroids, acetaminophen, and warfarin, can interact with alcohol, meaning that people with lupus may need to limit their alcohol intake to protect the liver and stomach. Taking some drugs, such as certain immunosuppressants, means that patients cannot consume alcohol at all.36 Patients should consult with a healthcare professional to better understand potential drug interactions.
Lupus is a global disease that affects an estimated 5 million people worldwide, with 16,000 new cases being discovered per year in the United States alone.2 Its prevalence varies significantly between regions. Over the past several decades, researchers have found the highest prevalence and incidence of SLE specifically in North America, with the lowest incidences reported in Africa and Ukraine. The lowest prevalence has been found in Northern Australia.38 Although data is limited, SLE specifically is reported to be more common and severe among people of African and Asian descent who reside in industrialized countries.39

One study assessed communication among patients with lupus and providers, using the following information:
After comparing information from different racial groups, researchers found that African Americans who had serious cases of lupus reported rushed communication with their healthcare providers. Moreover, African Americans who said their healthcare providers communicated poorly also had more lupus-related damage—a finding they did not share with white patients. The same study found that younger white people experienced less lupus-related damage than their Black counterparts.40
Lupus cannot be caught or spread. It is not transmissible through sexual contact, either. The virus is the product of several factors, including the environment, hormones, and genetics.41
If left untreated,or in patients with frequent and very severe symptoms, lupus can cause life-threatening problems. However, if patients receive consistent treatment and follow-ups, as many as 90% can expect to live a normal life.42
Lupus is not a type of cancer, but research indicates that people with lupus have a slightly heightened risk of developing cancer compared with people who do not have lupus. For example, for people with lupus, the risk of developing non-Hodgkin's lymphoma is four times that of people who do not have lupus. At the same time, it's associated with a decreased risk of other cancers, including breast cancer.43
No. Lupus is a chronic disease, and it does not go away on its own. However, effective treatments can lessen symptoms and minimize complications. A notable exception is drug-induced lupus, which usually disappears after the drug is stopped (if this is possible). Research to determine a cure for lupus is underway.44
Following general nutrition tips has overall health effects that can benefit anyone with lupus. Talk with a doctor or nutritionist to find a plan that best fits the symptoms of your disease and your specific nutritional needs.36,37
Explore lupus clinical trials at ClinicalTrials.gov.
Area of Focus: Inflammation & Immunology
Lupus is a focus of Pfizer’s Inflammation & Immunology Therapeutic Area. Visit the Inflammation & Immunology Page.
The information contained on this page is provided for your general information only. It is not intended as a substitute for seeking medical advice from a healthcare provider. Pfizer is not in the business of providing medical advice and does not engage in the practice of medicine. Pfizer under no circumstances recommends particular treatments for specific individuals and in all cases recommends consulting a physician or healthcare center before pursuing any course of treatment.