Are You at Risk for a Blood Clot?
NBC News war correspondent David Bloom was the image of health. In 2003, he was a 39-year-old avid tennis player. His work brought him to Iraq, where he was embedded with the 3rd Infantry Division, advancing toward Bagdad. Ultimately, it wasn’t the war, but a blood clot that killed Bloom, according to a TODAY.com account of his death.1
One night, he went to sleep out under the stars on a tank fender. He called his wife, Melanie, and mentioned that he had leg cramps. The symptom appeared natural, considering he had spent days on the road to Bagdad. A few days later, he was gone.2
A pulmonary embolism (PE) had lodged in his lungs, stopping the flow of blood. The clot stemmed from a condition called deep-vein thrombosis (DVT). A constellation of factors put Bloom at risk of this blood clot. Bloom had endured prolonged periods of immobility riding in cramped Army vehicles for long stretches. He'd experienced dehydration, which is common under the scorching Iraqi sun. He had taken a long-haul flight to the war zone. And he was a carrier of Factor V Leiden, a genetic mutation of blood-clotting factors that may increase the risk of blood clots in the legs or lungs.3
While Bloom’s death was tragic, his wife Melanie took solace in the fact that it raised the profile of blood clots, pulmonary embolism, and deep-vein thrombosis. She went on to become a spokesperson for the Coalition to Prevent Deep Vein Thrombosis. By sharing her husband’s story, she continues to shed light on the dangers of these conditions.
So, who’s at risk for a blood clot, and why?
Understanding Blood Clots
The Centers for Disease Control and Prevention (CDC) estimates that 900,000 Americans experience a deep vein thrombosis (DVT) or pulmonary embolism (PE) type of blood clot each year. That’s more than the annual number of heart attacks or strokes. Blood clots kill about 100,000 Americans each year.4
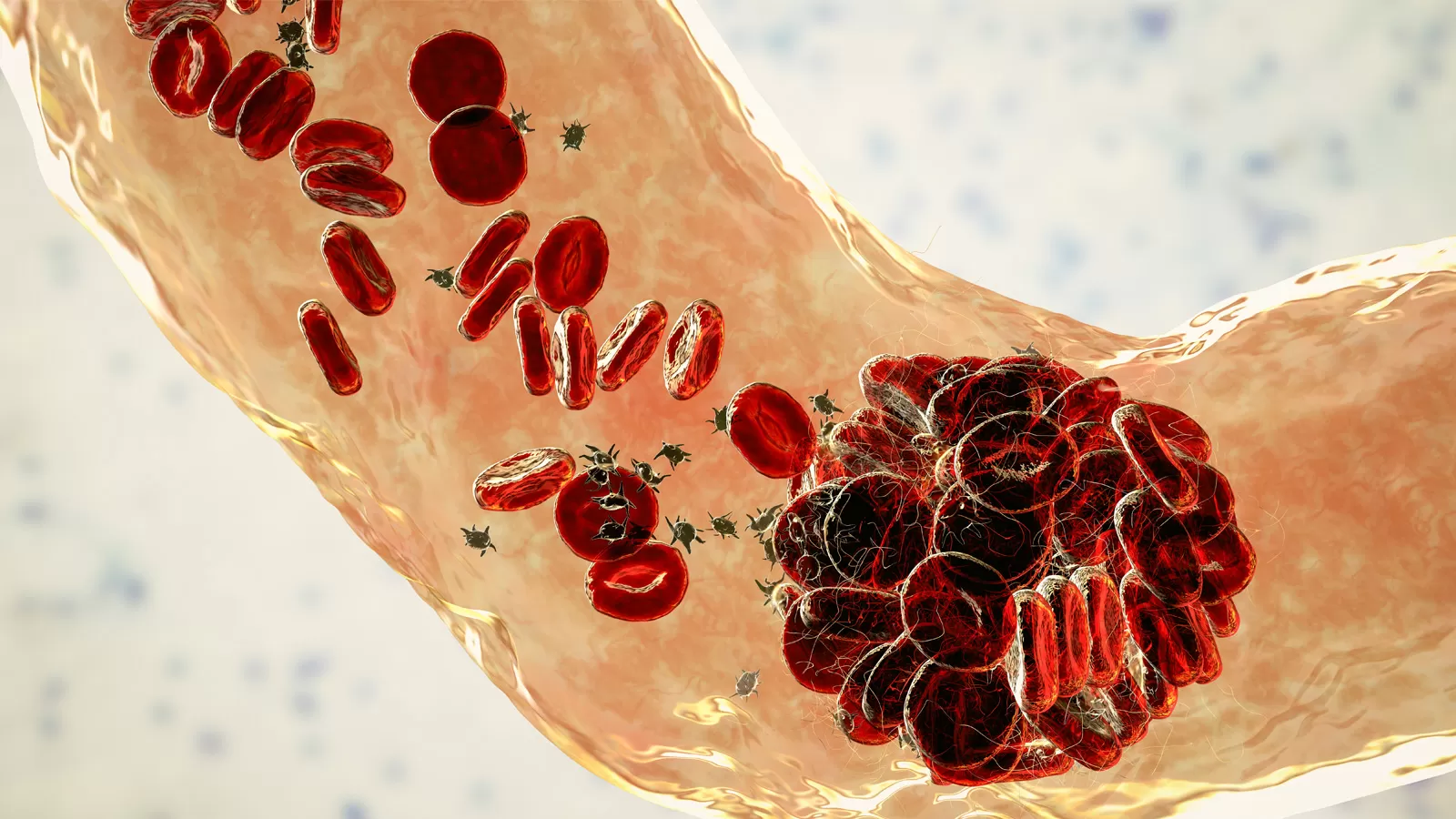
DVTs and PEs are collectively called a venous thromboembolism (VTE) and can occur singly or together. To break that down to its two parts, a thrombus is a blood clot at the specific place in a blood vessel where it starts. An embolus is when part or all of the clot moves elsewhere in the blood vessel. The largest concern about DVTs is they can progress to become a PE and be fatal, as they did with David Bloom.2,5
In DVT, a blood clot forms in a deep vein, typically in the pelvis, thigh, or arm. Deep-vein thrombosis can lead to a pulmonary embolism when a blood clot breaks off and obstructs blood vessels coming into the lung , decreasing the lung's ability to receive oxygen.2,5 This was the case with Bloom.2
Who Is at Risk of a Blood Clot?
There are risk factors for blood clots beyond what Bloom faced. They fall into categories called Virchow’s Triad, named after the Prussian doctor who discovered them. The three categories are blood stasis, hypercoagulability, and vascular injury. The more criteria a person meets, the higher their risk of a blood clot.6
In blood stasis, blood flow slows or pools.6 This is likely what happened to Bloom when he was riding in cramped Army vehicles or flying to Iraq. Other causes include long periods of bed rest following surgery, injury, or paralysis.7
Hypercoagulability occurs when blood becomes too sticky. Increased estrogen levels from birth control, pregnancy, or hormone replacement can lead to hypercoagulability. So can smoking.8 In Mr. Bloom’s instance, dehydration would render his blood more likely to clot or be more coagulable (hypercoagulable).
Finally, in trauma or vascular injury, a broken bone, major surgery, or soft-tissue injury damages blood vessels, increasing the chance of creating clots.9
An elevated risk for blood clots, deep-vein thrombosis, and pulmonary embolism exists for knee or hip surgery patients, patients with heart disease or low mobility after medical emergencies or procedures, and cancer patients, including those receiving chemotherapy, those who have broken bones or active infections, those who have experienced previous deep-vein thrombosis or pulmonary embolism, or anyone age 60 or older.9,10
Spotting Blood Clots
Certain signs and symptoms can indicate possible DVT or PE. In deep-vein thrombosis, about half of people experience no symptoms. Others have symptoms such as leg swelling, pain, tenderness, and redness at the site of origin.10 Similarly, pulmonary embolism can occur with or without symptoms and can be challenging to diagnose. Patients may experience very low blood pressure, cough up blood, have chest pain that worsens with deep breaths, an irregular heartbeat, or difficulty breathing. People with pulmonary embolism may also have a low-grade fever or a pulse that exceeds 100 beats per minute.11
If you notice any of these blood clot signs or symptoms, act quickly. Seek immediate medical help. Deep-vein thrombosis and pulmonary embolism require a doctor’s diagnosis and care. A PE, or pulmonary embolism, requires immediate medical attention.
Treating and Preventing Blood Clots
On the advance to Baghdad, Bloom was a world away from the care he needed. When he awoke after his night on the tank fender, he seemed to be in better spirits, his wife said. Without proper medical intervention, however, he collapsed and died a few hours later.12,13
At the first sign of deep-vein thrombosis, doctors will start treatment to lower the odds of a clot breaking loose and entering the bloodstream, where it can lodge in the lungs and cause a pulmonary embolism. Typically, physicians use medicines called blood thinners, which help stop clots from growing. Sometimes, surgeons operate to remove clots or administer medicines called thrombolytics to break up clots.14 Pulmonary embolism cases often require thrombolytics, surgery, and blood thinners after the procedure.15
Even after a blood clot emergency ends, the work of managing blood clots continues. Healthcare teams often prescribe medications and recommend lifestyle modifications to help decrease the risk of future blood clots. Adherence to the treatment plan is critical.16
The best ways lower your risk of venous thromboembolism, deep-vein thrombosis, and pulmonary embolism are to quit smoking, lose weight (as obesity is another blood clot risk factor), stay hydrated and active, and exercise to decrease the chance of blood stasis and hypercoagulability.16,17
The impact of blood clots extends beyond the patient. Bloom’s death forever changed the lives of his wife and three young daughters. But with sufficient understanding of the science, blood clots are a tragedy many people can avoid.
![]()






