Getting a Medicine to the Brain Is a Major Challenge in Drug Design: How This Scientist Solved It
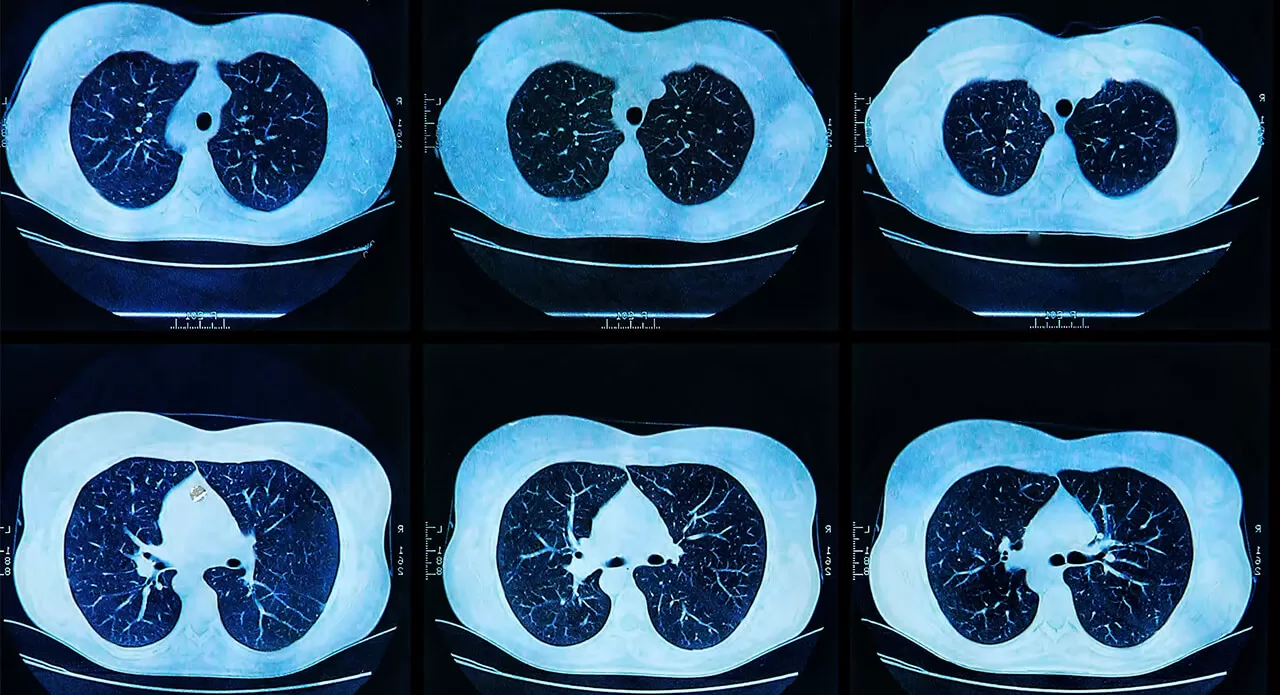
For cancer patients who have been treated with a particular medicine for some time, one of the hurdles many of them face is the tumor developing a resistance to the medicine. It’s a cruel twist that can affect patients being treated for non-small cell lung cancer, which can mutate and begin attacking the brain.
Lung cancer accounts for most cancer-related deaths in the U.S., with non-small cell lung cancer being the most common type,, so the scope of the problem is broad.
But if lung cancer does metastasize into the brain, finding an appropriate cancer-fighting drug can be an immense challenge because of the blood-brain barrier, the thin barrier of tightly packed cells that protects the brain from harmful pathogens and other substances that may disturb the brain’s delicate chemical balance. This barrier is impenetrable to nearly 95 percent of medicines.

"There’s nothing better than designing a molecule and making it and then finding out it’s active against whatever target you’re looking at," says Ted Johnson.
Finding a solution for this formidable problem was what faced chemist Dr. Ted W. Johnson, who joined Pfizer in 2001 after his own mother’s cancer-related death while he was a post-doc at Harvard prompted him to pursue a career developing cancer medicines.
“In the end, I said, ‘I'm going to go into industry because this is where I want to have an impact on patients, and I want to work on medical needs,’” says Johnson, who’s now a Research Fellow in Oncology Medicinal Chemistry at Pfizer’s R&D site in La Jolla, California.
Johnson played a pivotal role in designing an innovative medicine now being tested for patients with non-small cell lung cancer whose tumors have metastasized into the brain. The breakthrough achieved by Johnson and his fellow “drug hunters” was aided by high-tech tools that allows them to visualize drug molecules and their target receptors in 3-D and enables them to manipulate them in virtual reality.
Architecting New Drug Molecules in 3-D
Much like architects might examine a potential construction site via 3-D maps, three or four drug designers will work as a team in a room with a few 55-inch flat-screen TVs, Johnson says, looking at the molecules projected on the TV, and rotating them in three dimensions. Among the 3-D visualization tools that Johnson and his team uses is a program called MoViT (Molecular Visualization Tool), which can play a vital role in developing medicines, particularly when scientists need to tweak the structure of an existing medicine.
“Every molecule has a 3-D shape and you want to change that shape to bind to a particular target,” Johnson explains. “It's like a lock and key.”
“You can view all of this in three dimensions. We can view the drug bound to the protein, and then change it and put it back in and see how well it does in the computer,” he adds. “It's really impressive. We use structure-based drug design a lot.”
To solve the problem of trying to create an anti-cancer drug molecule that can pass through the blood-brain barrier, Johnson and his team used 3-D visualization tools to modify an existing U-shaped drug molecule into a spherical molecule.
“It doesn't seem like a big difference, but if you make the compound really spherical and rigid like a ball, it makes it easier for the molecule to pass through the blood-brain barrier,” Johnson says. “The loose ends of the U-shaped molecule wiggle around and get tangled up in the blood-brain barrier.”
This solution, while simple in retrospect, involved his team’s collective resources and brain power focused on this problem for some four years, which was actually an accelerated timeline, Johnson notes.
A Delicate Balancing Act
Another area in which 3-D visualization tools can play an important part is in making the molecule more selective, which can reduce unwanted side-effects of medications. If this issue arises, the designer has to change the shape of the drug molecule, “but not change it too much that it doesn't bind to your target. So, that's a balancing act,” Johnson says.
For researchers like Johnson, the ability to manipulate molecules in three dimensions has been a major boon, as well as professionally gratifying. “There’s nothing better than designing a molecule and making it and then finding out it’s active against whatever target you’re looking at,” Johnson says. “It’s exciting and it’s completely new.”